Dry eyes and dry mouth are the characteristic symptoms of Sjögren’s – a chronic autoimmune disease affecting the body’s moisture-producing glands and membranes.
However, one oft-underreported and under-discussed symptom of Sjögren’s is hair loss. Like other autoimmune conditions that attack the healthy cells in the body (which include hair follicles), this syndrome can also cause alopecia.
But that’s not the only way in which it affects the hair. Since Sjögren’s affects the body’s ability to produce a normal amount of moisture, it also affects the body’s largest organ – the skin.
Dry skin is another symptom of this condition. And when the skin is dry, so is the hair attached to it, which further exacerbates the problem. It also doesn’t help that scarring (cicatricial) alopecia is also associated with autoimmune diseases. Still, there might be a few treatments that can help you. Read on to learn more.
Can Sjögren’s Cause Hair Loss?
Being an autoimmune condition, Sjögren’s syndrome can cause hair loss.
Mainly, it affects the salivary glands in the mouth and the lacrimal (tear) glands in the eyes.
However, it can also affect other organs of the body, such as the:
- Joints
- Kidneys
- Lungs
- Nerves
- Blood vessels
- Digestive organs
Additionally, among other parts of the body, it affects the skin, resulting in a condition known as xeroderma.
That can cause a burning sensation, itchiness, dry skin, and dry hair. The hair’s not just dry, it’s also dull-looking because it lacks shine (that comes from moisture).
Here, it should also be noted that there are two types of Sjögren’s syndrome:
- Primary Sjögren syndrome – Sjögren’s is considered primary when it occurs alone without any other rheumatic disease (autoimmune or inflammatory disease affecting the joints, muscles, ligaments, bones and tendons).
- Secondary Sjögren syndrome – Sjögren’s is considered secondary when it coexists with other rheumatic autoimmune diseases like rheumatoid arthritis, scleroderma, lupus or primary biliary cholangitis.
Now, because Sjögren’s can occur with other autoimmune conditions, it can’t always be held primarily responsible for hair loss.
For instance, in the case of rheumatoid arthritis, other types of hair loss, like alopecia areata and telogen effluvium can occur together. So, it’s not always easy to pinpoint the actual cause of hair loss.
In fact, as Sjögren’s usually begins around menopause, your doctor might misdiagnose it altogether since menopause may also cause dry eyes, dry mouth, and hair loss.
What Causes Sjögren’s Hair Loss?
The link between Sjögren’s and hair loss is not well studied. However, there are different mechanisms in which it may be doing so.
Immune Cells Attack
One of the ways in which Sjögren’s can cause hair loss is the attack of the immune cells on the healthy hair follicles. In turn, this attack can result in the loss of hair.
Those suffering from this condition report noticeable hair loss with bald spots forming on the scalp. You might notice it when combing your hair, washing it or when you run your fingers through it.
Side Effect Of Medication
The medicines used for the treatment of Sjögren’s can also end up causing hair loss (it may also be due to the syndrome itself and the medicine).
Hydroxychloroquine, sold under the brand name Plaquenil, is sometimes prescribed for the treatment of Sjögren’s symptoms. However, according to RxList, hair loss is one of the common side effects of this drug.
Methotrexate is another drug that’s used for suppressing the immune system in autoimmune conditions. It may be prescribed for Sjögren’s too. And unfortunately, this drug can also cause hair loss as a side effect.
Additionally, hair loss can also be caused by drugs like rituximab and prednisone prescribed for Sjögren’s syndrome.
Frontal Fibrosing Alopecia
There are different case studies that report an association between frontal fibrosing alopecia and Sjögren’s syndrome.
A survey published in Cutis found that many patients with frontal fibrosing alopecia had a history of autoimmune diseases. Of the 29 patients that were a part of the study, 3% of them had Sjögren’s.
Frontal fibrosing alopecia is a type of scarring alopecia that permanently damages the hair follicles and replaces them with scar tissue.
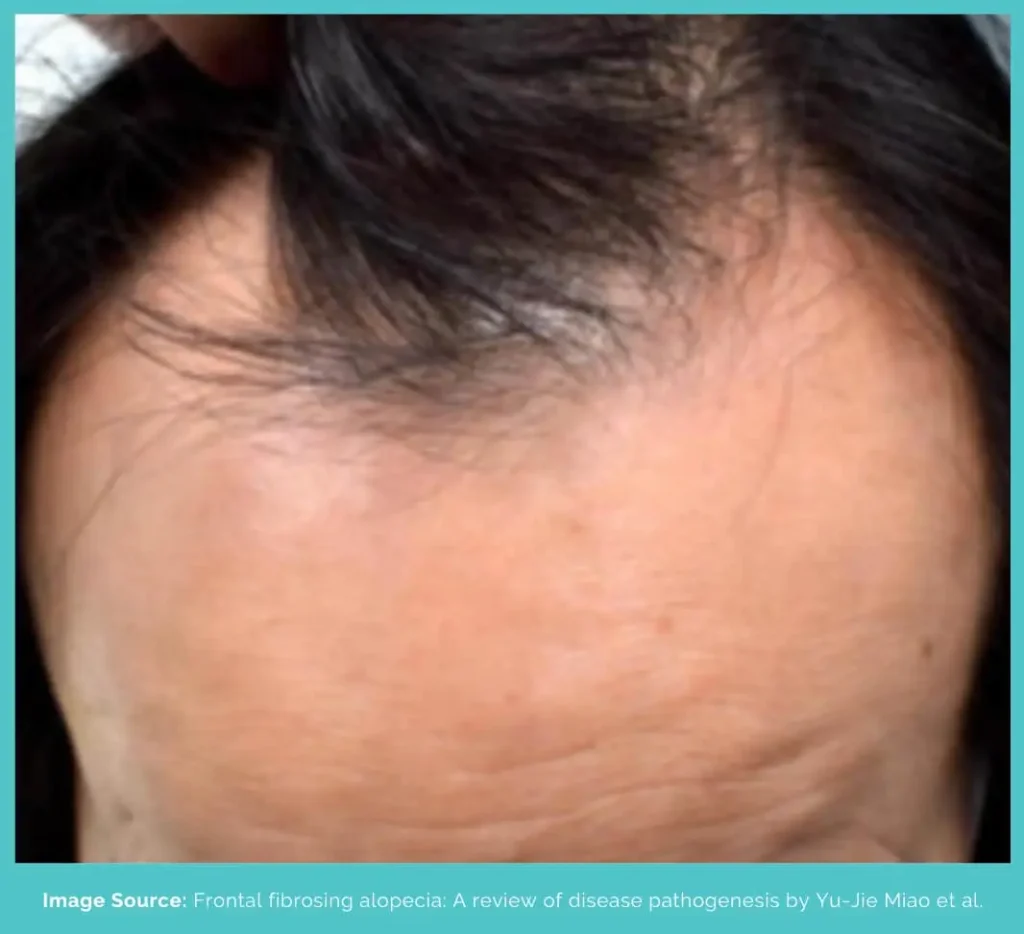
Its characteristic feature is the band-like loss of hair at the front of the scalp. But it can cause loss of hair on the face and body.
Stress
Needless to say, living with Sjögren can be stressful. And the stress can trigger a type of hair loss known as telogen effluvium. It’s when the hair leaves the growing (anagen) phase and enters the resting (telogen) phase instead. And that results in the shedding of hair.
Another thing that may stress the body is the medications of Sjögren’s. For instance, immunosuppressants are prescribed for this syndrome.
And immunosuppressants can make you more prone to illnesses (even a cold). Bear in mind that the shock of an illness can also trigger telogen effluvium.
Dryness
Dryness resulting from Sjögren’s can cause make the hair brittle and prone to breakage.
Sebum not only moisturises and hydrates the hair but also protects it from breaking too easily.
However, since this syndrome can affect the oil-producing glands in the body, it can make the hair drier, making it break more easily.
Is Sjögren’s Hair Loss Permanent?
Sjögren’s hair loss can be permanent if you’ve developed scarring alopecia.
There are anecdotal reports of people using different oils (castor, argan, coconut, etc.) and supplements to grow their hair back while suffering from Sjögren’s.
However, you should consult your doctor before investing your time and money in these. That’s because they might not do anything for you.
What’s The Treatment For Sjögren’s Hair Loss?
The treatment for Sjögren’s hair loss will depend on the kind of hair loss you’re suffering from.
If you’ve frontal fibrosing alopecia, you might be prescribed corticosteroids, finasteride, minoxidil, hydroxychloroquine (it’s also used for treating hair loss) or even laser therapy.
You might also be recommended the use of biotin supplements (take them if advised by your doctor). Other than that, controlling the symptoms of the condition itself may also have a positive impact on your hair.
Conclusion
Sjögren’s is not an easy condition to live with. Aside from its many problematic symptoms, hair loss can be a source of additional concern. And while this symptom is often dismissed, it can cause significant distress to the person experiencing it.
Unfortunately, it may not always be possible to reverse this type of hair loss. In that case, you can consider wearing wigs, hats, scarves or getting micropigmentation to cope with the hair loss.
But before anything, you should first get in touch with an experienced and board-certified medical professional.
Dr Cagla
Dr Cagla earned her medical degree at Trakya University’s Faculty of Medicine in Bulgaria and has almost 6 years of hair transplantation experience. She is a specialist in FUE, DHI and Sapphire hair transplants of the scalp, eyebrows and beard and has performed over 6,000 surgeries. Dr Cagla is multilingual, with fluency in English, Bulgarian and Turkish.
