
Alopecia areata is a chronic, autoimmune condition. It is an unpredictable disease in which the immune system attacks healthy hair follicles, resulting in hair loss. In this guide, you’ll learn more about what alopecia areata is, why it might occur and what can be done to treat it.
What Is Alopecia Areata?
Alopecia areata is an autoimmune disease in which the immune system malfunctions, resulting in chronic, non-scarring hair loss. It is believed to be triggered by genetic and environmental factors.
French physician and nosologist François Boissier Sauvages de Lacroix first used the term “alopecia areata” in 1763 in his book “Nosologia Methodica.” “Alopecia” means fox in Greek (due to the loss of fur seen in fox mange). “Areata” is derived from Latin, meaning a vacant area or a patch.
Typically, this type of hair loss results in bald patches, although it can also be diffuse. It can affect any hair-bearing part of the body, face or scalp — there can be spontaneous remissions and then relapses. Fortunately, alopecia areata doesn’t destroy the hair follicle. The stem cells remain intact, which is why regrowth is possible months or even years after an episode has occurred.
Both children and adults can be affected by this condition. In children, however, the disease is more likely to progress to more severe stages if they develop alopecia areata as early as 5 years of age or even younger, according to the National Alopecia Areata Foundation.
What Different Types of Alopecia Areata Are There?
There are 8 different types of alopecia areata, which are as follows:
Patchy Alopecia Areata – Characterised by the formation of one or more circular or oval-shaped bald patches, it is the most common type.
Alopecia Totalis – Refers to the complete loss of hair on the scalp.
Alopecia Universalis – Results complete hair loss occurs on the scalp, face and body.
Alopecia Barbae – Causes patchy or diffuse (rarely) hair loss in the beard region.
Alopecia Incognita – Seen as diffuse hair loss accompanied by the formation of yellow dots (sebum or keratinocytes) and miniaturised hair.
Ophiasis – Comes from the Greek word for “snake” because of its wave-like appearance. It occurs at the circumference of the head (occipital and temporal regions).
Sisaipho (Inverse Ophiasis) – Results in loss of hair on the centre of the scalp. The temporal and occipital regions are spared.
Marie Antoinette Syndrome – Alluding to the French Queen whose hair turned white before the last walk to the guillotine. It is characterised by hair turning white overnight with diffuse alopecia.
How Do You Know If You Have Alopecia Areata?
The most common sign of alopecia areata is the sudden loss of hair in circular patches. These patches have distinct borders and are smooth to the touch, and they can increase in size (even unite with the other patches). Usually, hair loss starts on the scalp, but it can progress to the face (eyebrows, eyelashes, inside the nose, beard) and other areas of the body (armpits, pubes, legs, chest, stomach). A few researches report slight swelling in the lesions with no other signs of inflammation (like redness or pain).
A type of hair dystrophy has also been observed where the hair takes the shape of an exclamation point – narrower at the base. Such hairs are usually seen at the borders of the patches. According to the American Academy of Dermatology, “itching, tingling or a burning sensation” may also occur in the affected area — before the beginning of the hair loss or afterwards.
Other than that, alopecia areata can also be accompanied by nail changes. According to a study published in the Journal of the European Academy of Dermatology and Venerology, nail abnormalities have been observed in 10-66% of the patients with alopecia areata. For instance, it can cause the following:
- Fine pitting
- Trachyonychia (sandpapered, thin and brittle nails)
- Ridges
- Red nails
Alopecia areata can also affect the eyes. For instance, it can affect the function of the retinal pigment epithelium (pigmented layer over the retina).
How Common Is Alopecia Areata?
Alopecia areata affects about 2% of the general population. This is the second most common type of non-scarring alopecia after androgenetic alopecia.
Women and men are affected equally, but it’s been reported that it affects more Africans than Asians and Caucasians.
When Does Alopecia Areata Start?
Alopecia areata can occur at any age but research shows that its incidence increases with age.
According to a study published in Clinical, Cosmetic and Investigational Dermatology, 40.2% of people get alopecia areata by 20 and 82.6% to 88% of them by the time they reach 40 — the mean onset age being somewhere between 25 and 36.
However, it can also occur in children and early-onset can mean the development of more severe types of alopecia areata.
How Long Does Alopecia Areata Last?
An episode of alopecia areata can last for a few months to even years. It’s possible for hair loss and hair regrowth to occur simultaneously – new patches form as hair grows in the old ones. If you’re able to pull your hair out easily, it means that your alopecia areata is still active, according to the American Osteopathic College of Dermatology.
A review published in the International Journal of Trichology reported that around 34-50% of people recover within one year, but in 14-25% of the cases, alopecia areata worsens to alopecia totalis or universalis, and in the latter cases, full recovery isn’t as likely to occur.
What Causes Alopecia Areata?
It’s not exactly understood what causes alopecia areata. However, it’s believed to occur due to genetic and environmental factors.
As far as genetics are concerned, variations in the human leukocyte antigen (HLA) gene are thought to make people susceptible to this disorder.
This HLA complex helps the immune system in differentiating between the body’s own and foreign proteins. When there’s a problem with that, the body can start attacking its own healthy cells (like the hair follicles). Still, it’s a polygenic trait – other genes also play a role in the development of alopecia areata.
It’s also worth noting that this type of hair loss tends to run in families. Congenital alopecia areata has been reported. Reported triggers also include infections, vaccinations, illness, drugs, and emotional and physical distress.
Other than that, since alopecia areata is autoimmune, it’s also been associated with other autoimmune conditions, such as:
- Graves’ and Hashimoto’s
- Lupus
- Type 1 diabetes
- Pernicious anaemia
- Vitiligo
- Celiac disease
- Psoriasis
- Rheumatoid arthritis
- It’s also been associated with allergic conditions like hay fever (allergic rhinitis), eczema, asthma, and allergic conjunctivitis.
Other comorbidities of this disorder include anxiety, depression, and vitamin D deficiency, among others.
How Do You Test For Alopecia Areata?
Testing for alopecia areata usually involves dermoscopy. A handheld device is held to the surface of the skin for a closer examination.
During this, doctors usually look for any black or yellow dots, exclamation point hairs and broken hairs.
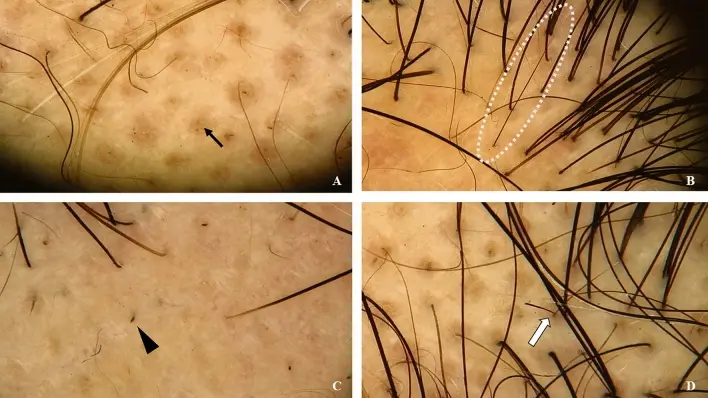
A Yellow Dot: Black arrow… B Erect and Regenerated Hairs… C Black Dot: Black triangle… D Exclamation Mark Hair. Xu W, Xie B, Wei D, Song X. Dissecting hair breakage in alopecia areata: the central role of dysregulated cysteine homeostasis. Amino Acids. 2024 May 21;56(1):36. doi: 10.1007/s00726-024
A hair pull test might also be done to assess if active hair loss is taking place. Additionally, blood tests might be done to rule out any deficiencies or hormonal imbalances.
Of course, questions about your lifestyle and general health will also be asked in addition to your medical history.
Your doctor may also perform a scalp biopsy to rule out any other similarly-presenting alopecias.
Can Alopecia Areata Be Treated?
Currently, there’s no cure for alopecia areata. However, there are different treatments that may help. Still, you must bear in mind that not a lot of the treatments are effective or result in long-term regrowth.
Steroids
Steroids are the most commonly prescribed medications for alopecia areata. These can be:
- Topical Steroids (lotion or shampoo) – Work best for mild cases and are usually applied for 3-6 months.
- Intralesional Steroids – Are injected into the alopecia areata lesions, so only treat one area. These are also not suitable for the more aggressive types.
- Oral Steroids – Work best for more aggressive alopecia areata.
Your doctor will decide which one will work best for you.
Contact Immunotherapy
Topical immunotherapy or contact immunotherapy is a type of technique in which the skin of the scalp is exposed to an allergen. This, in turn, induces an allergic reaction, which helps with hair regrowth.
Research published in JAMA Dermatology reported that contact immunotherapy resulted in minor regrowth in 64.9%, major regrowth in 56.1%, and complete regrowth in 42.6% of patients with patchy alopecia areata.
JAK Inhibitors
Different researches have shown that JAK inhibitors — which inhibit the activity of certain enzymes to reduce inflammation — can also help with alopecia areata.
The US FDA has also approved three JAK inhibitors for the treatment of severe alopecia areata, which are as follows:
- Olumiant (baricitinib)
- Litfulo (ritlecitinib)
- Leqselvi (deuruxolitinib)
One problem with these drugs, however, is that there’s a high chance of recurrence after these drugs are discontinued. Also, JAK inhibitors can cause some serious side effects, such as infections, high cholesterol, and cardiovascular issues.
PUVA Phototherapy
Psoralen + ultraviolet light A therapy, also known as photochemotherapy, involves the topical application or ingestion of the light-sensitive drug: psoralen. It is done 2-3 times every week for months to treat alopecia areata.
However, the problem with this treatment is also that it has a high relapse rate. Additionally, it can also cause some serious side effects, one of which is squamous cell skin cancer.
Immunosuppressants
Since alopecia areata is an autoimmune disease, one treatment option is immunosuppressants (methotrexate and cyclosporin). But this is reserved for more severe types of alopecia.
Infection is a very major risk of taking immunosuppressants, so the benefits have to be weighed against the risks before the prescription.
Others
Because low zinc and vitamin D levels have been observed in patients with alopecia areata, you might be recommended their supplements by your healthcare facilitator. They might be given in combination with other drugs.
Other than that, prostaglandin F2α analogues and anthralin are prescribed in certain instances. For instance, the former is to help with the regrowth of eyelashes.
What Not To Do With Alopecia Areata?
When you have hair loss due to alopecia areata, it’s important to take good care of your hair and scalp by doing things such as:
- Avoiding tight hairstyles
- Using gentle hair care products
- Limiting the excessive use of styling tools (e.g. blow dryers and hot rollers)
- Consuming anti-inflammatory foods (e.g. fruits, nuts and leafy greens)
- Managing stress
- Keeping the scalp protected from the harmful UV rays of the sun
In any case, if you have alopecia areata, it is of the utmost importance that you seek professional help.
Does PRP Work For Alopecia Areata?
Different case studies and small researches show the promising potential of platelet-rich plasma (PRP) injections for alopecia areata.
A double-blind, placebo-controlled study published in the British Journal of Dermatology showed that PRP increased hair regrowth and decreased hair dystrophy (along with burning or itching sensations) in patients with alopecia areata.
It does, however, require more research. So, you should consult a medical professional before considering it.
Can Minoxidil Help With Alopecia Areata?
Minoxidil is commonly prescribed to alopecia areata patients to promote hair regrowth. It won’t, however, treat alopecia areata itself as it doesn’t help with inflammation. Still, it can help in regrowth by increasing flow of the nutrients and oxygen to the hair follicles.
Can Hair Transplant Help Alopecia Areata?
Since alopecia areata is a chronic, autoimmune condition, you’re not likely to be a candidate for this surgery.
Hair transplant surgery takes follicles from the back and sides of the head and implants them in the balding regions.
With alopecia areata, no follicle on the scalp is safe from being attacked by the immune system, so you can end up losing the transplanted hair.
Depending on how extensive the condition is, you might not even have enough donor area for the hair transplantation to take place.
Even if your surgeon is willing to perform a hair transplant, the success rate will likely be quite low.
Can Alopecia Areata Be Reversed?
Since alopecia areata only affects the hair bulb, it’s usually reversible. Hair is able to regrow due to the hair follicle stem cells. However, this only happens once the inflammation has subsided.
During regrowth, you may notice some hair changes. For instance, your hair might feel fine and less pigmented (white or greyish) than before. Fortunately, this isn’t permanent. Your hair will regain its original colour and thickness.
Still, it’s not possible to predict exactly when what will happen. Hair regrowth after alopecia areata can be full or partial (hair loss can be permanent), and it usually happens in a few months.
How To Avoid Alopecia Areata?
Because it is not understood what causes alopecia areata in the first place, it is also unclear how to prevent it.
You can try avoiding some of the triggers that are believed to cause this condition.
For instance, stress may lead to an episode of alopecia areata, so you can try doing different things (meditation, deep breathing, yoga, seeking professional help) that can help you manage it.
But keep in mind that it’s not always possible. Alopecia areata can even occur in completely healthy people.
How To Cope With Alopecia Areata?
Alopecia areata may not be life-threatening but it can impact the overall quality of life.
Loss of hair due to alopecia areata can make people feel anxious and depressed. It can also lead to social isolation.
Getting professional help or joining patient support organizations (like Alopecia UK) can help. However, for many people, concealing hair loss is one way to cope with this.
How to Hide Alopecia Areata?
Wigs and hairpieces can help hide hair loss on the scalp due to alopecia areata. Additionally, hair fibres can camouflage the scalp if you have bald patches.
You can also choose to completely shave your head, or you can get a buzzcut look with scalp micropigmentation. Some people may consider wearing scarves, caps, and bandanas to help with it.
For the face, makeup, false lashes, and microblading could be helpful. Wearing huge shades may also be effective in concealing eyelash and eyebrow hair loss.
Frequently Asked Questions
Alopecia areata progresses quite quickly. Hair loss occurs suddenly, and patients develop bald patches on their scalps in a matter of weeks.
In order to stop the spread of alopecia areata, you must get in touch with a medical professional and seek appropriate treatment, which can include medications like steroids or JAK inhibitors. Still, it’s important to bear in mind that treatments don’t always work, so there’s no guarantee that you might be able to stop alopecia areata from spreading.
Alopecia is a chronic condition, so it can come and go. However, there are some people who only ever have one episode of this condition.
The relationship between alcohol consumption and alopecia areata is not exactly clear. However, some research suggests that alcohol can increase the risk of alopecia areata.
To our knowledge, there’s no scientific evidence that suggests that coffee can cause alopecia areata.
The Severity of Alopecia Tool or SALT, as the name suggests, is used to measure the severity of alopecia areata. It does so by dividing the scalp into 4 sections, according to the size of their respective areas. The percentages are then added to get a final score.
One case study published in JAAD Case Reports details the case of a patient who developed alopecia totalis after the use of permanent hair dye; it was treated. However, there’s not much evidence of the association between the two.
Dr Cagla
Dr Cagla earned her medical degree at Trakya University’s Faculty of Medicine in Bulgaria and has almost 6 years of hair transplantation experience. She is a specialist in FUE, DHI and Sapphire hair transplants of the scalp, eyebrows and beard and has performed over 6,000 surgeries. Dr Cagla is multilingual, with fluency in English, Bulgarian and Turkish.
